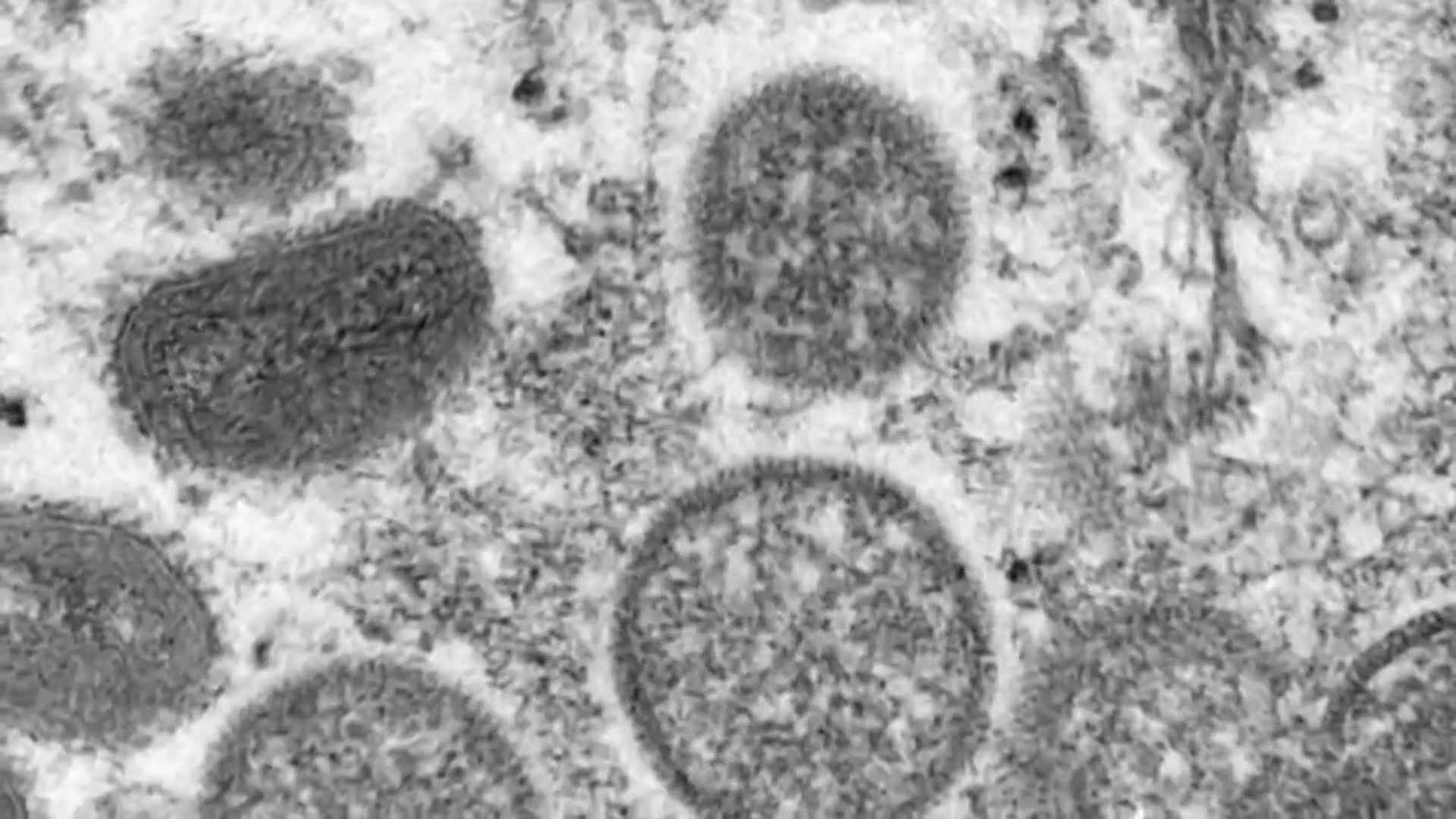
Reported cases of monkeypox are soaring in Illinois, with 533 cases recorded by the Centers for Disease Control as of Tuesday.
And according to the Chicago Department of Public Health, the majority of those cases come from Chicago.
The CDC shows that Illinois currently ranks as the state with the third-highest number of cases, following only New York, which has more than 1,600 cases, and California, which has more than 800 cases.
Such statistics led Gov. J.B. Pritzker on Monday to declare monkeypox a public health emergency, classifying the state as a "disaster area" in regards to the disease.
Feeling out of the loop? We'll catch you up on the Chicago news you need to know. Sign up for the weekly Chicago Catch-Up newsletter here.
While the declaration does allow officials to more easily secure monkeypox vaccine shipments and ramp up distribution, the vaccine is still only available from a limited -- albeit but growing -- federal stockpile. And, it's currently only being offered to those at "highest risk" of the virus.
Here's a breakdown of what that means, and what could change as the vaccine is slowly set to become more widely available.
Getting the Monkeypox Vaccine in Chicago
According to a July 27 update from the Chicago Department of Public Health, the monkeypox vaccine supply remains very limited, "though it is expected to continue to ramp up over the next few months as the U.S. acquires additional doses."
CDPH also noted that "Vaccine is only available from the national stockpile and federal partners distribute it to states and cities based on population and MPV case counts. Chicago received an additional 15,000 doses of the vaccine over the weekend, by far the city’s largest allotment to date."
"However," CDPH continued, "many more individuals want vaccine than can receive it."
In a Facebook Live update Tuesday, CDPH Commissioner Dr. Allison Arwady echoed this sentiment, but indicated that 13,000 more doses of the vaccine have been ordered.
"We have seen people waiting in line for hours," Arwady said, in reference to recent monkeypox vaccine events for eligible individuals. "We are trying very, very hard with all of the providers to instead get people appointments just to cut down on this standing in line. That is already getting better. And that tells us there's still a lot more demand than supply, so when this next batch gets here, which I expect in the next 1-2 weeks or so, we'll be pushing those out quickly."
CDPH says that is prioritizing the vaccine for those at "highest risk," which includes "any individual who has had close physical contact with someone diagnosed with MPV or whose sexual partner was diagnosed with MPV in the last 14 days."
And while Arwady noted that the city anticipates conducting larger vaccination events when more vaccine is available, there's still a backlog of those "highest risk" individuals who are first in line -- but that as vaccine supply improves, more individuals will become eligible to get it.
"In terms of exactly how the eligibility will open, I don't know for sure just yet, because we are still really seeing a lot of people with these highest risk factors filling up so and we want to see how the epidemiology of the of the disease is going."
According to public health officials, the full course of vaccine consists of 2 doses given at least 4 weeks apart. It takes about 2 weeks for the first dose to take full effect.
Getting Tested for Monkeypox in Chicago
According to Arwady, testing for monkeypox in Chicago is readily available, with or without health insurance through CDPH, at federally qualified health centers, or through your doctor's office.
"It all has to be done through a provider -- you cannot just go to a laboratory to get a test -- so give us a call if you're not sure where to go," Arwady said. "We will get you connected right away to a provider and work on getting you the testing that you need."
If you are looking to get tested for monkeypox in Chicago, you can call the public health department at 312-746-4835.
Those at Risk
While doctors have said that the overall risk to the general public remains low, with transmission is most often occurring from close personal or sexual contact -- WHO’s top monkeypox expert Dr. Rosamund Lewis last week said that 99% of all monkeypox cases beyond Africa were in men and that of those, 98% involved men who have sex with men -- the illness is spreading in ways that experts haven't seen before.
Still, doctors are stressing that says the virus des not discriminate.
“MPV is not a ‘gay disease’,” CDPH Commissioner Dr. Allison Arwady said. “There’s nothing inherent in the biology of the virus that limits it to men who have sex with men. The virus spreads through tight-knit social networks; it does not discriminate.”
According to the Chicago Department of Public Health, "Person-to-person transmission is possible through "close physical contact with monkeypox sores, items that have been contaminated with fluids or sores (clothing, bedding, etc.), or through respiratory droplets following prolonged face-to-face contact."
Arwady said most cases "are coming from much more intimate skin-to-skin contact or kissing" and noted that most casual contact and day-to-day activities - including things like shopping in crowded stores, going to a bar or coffee house, riding crowded CTA trains and buses, or using gym equipment or public restrooms - pose little to no risk for contracting MPV.
According to Dr. Albert Ko, a professor of public health and epidemiology at Yale University, “The bottom line is we’ve seen a shift in the epidemiology of monkeypox where there’s now widespread, unexpected transmission. There are some genetic mutations in the virus that suggest why that may be happening, but we do need a globally-coordinated response to get it under control."
Monkeypox Symptoms
The CDPH says Monkeypox is a rare, but potentially serious viral illness, which often begins with flu-like symptoms and swelling of the lymph nodes, and progresses to a rash on the face and body, health experts said.
Virus symptoms range from fever, aches and rashes all over the body.
"Suspected cases may present with early flu-like symptoms and progress to lesions that may begin on one site on the body and spread to other parts," CDPH previously stated.
Dr. Irfan Hafiz, an infectious disease specialist with Northwestern Medicine’s McHenry and Huntley hospitals, said the virus causes symptoms that are similar to several maladies, including chickenpox or smallpox.
“It can, to the layperson, look like chickenpox or warts,” he previously said. “But these (sores) tend to be in exposed areas.”
Health experts also stated the illness can be confused with a sexually transmitted infection like syphilis or herpes, or with varicella zoster virus.
In the U.S., some experts have speculated whether monkeypox might be on the verge of becoming an entrenched sexually transmitted disease in the country, like gonorrhea, herpes and HIV.
National Response
The Biden administration is considering declaring a nationwide public health emergency in response to the growing outbreak, but has yet to do so. Dr. Ashish Jha, the White House COVID response coordinator, said last week the administration was looking at how a public health emergency declaration might bolster the U.S. response to the outbreak.
“There’s no final decision on this that I’m aware of,” Jha said. “It’s an ongoing, but a very active conversation at HHS.”
Health and Human Services Secretary Xavier Becerra has the authority to declare a public health emergency under the Public Health Services Act. A declaration can help mobilize federal financial assistance to respond to a disease outbreak.
The World Health Organization last week activated its highest alert level, declaring the virus a public health emergency of international concern.