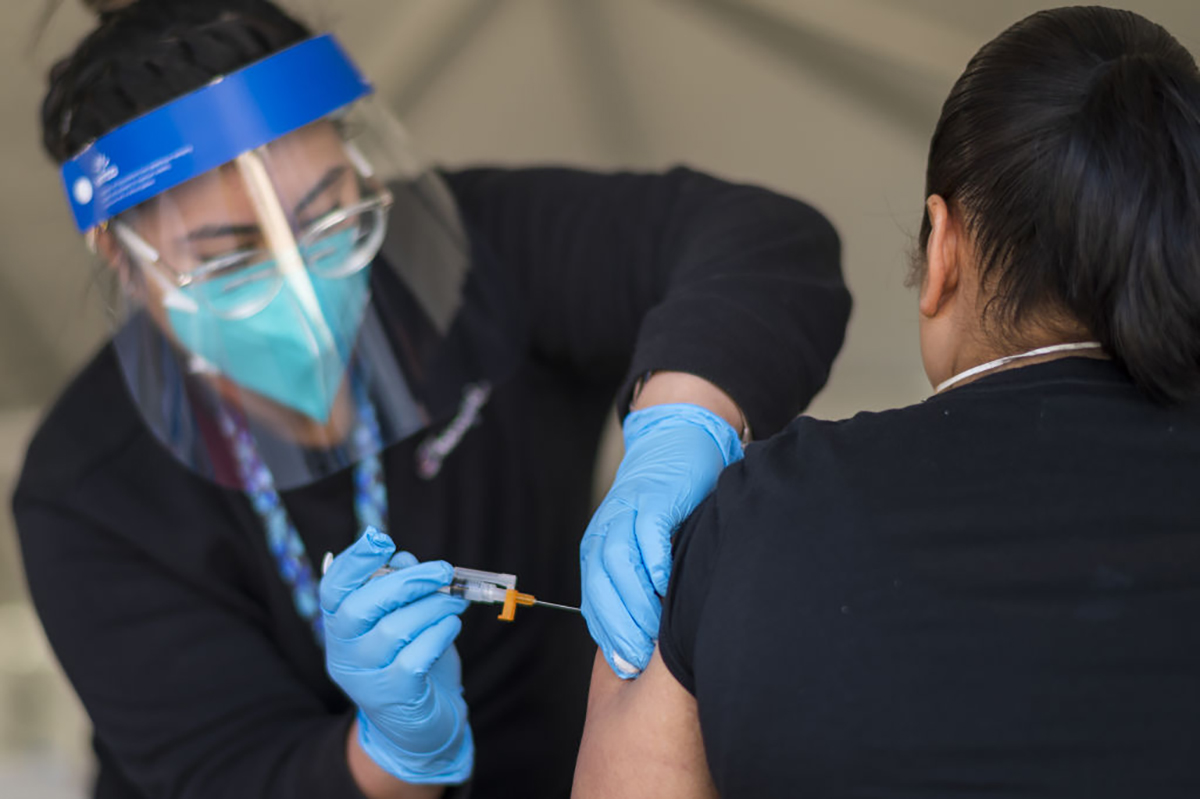
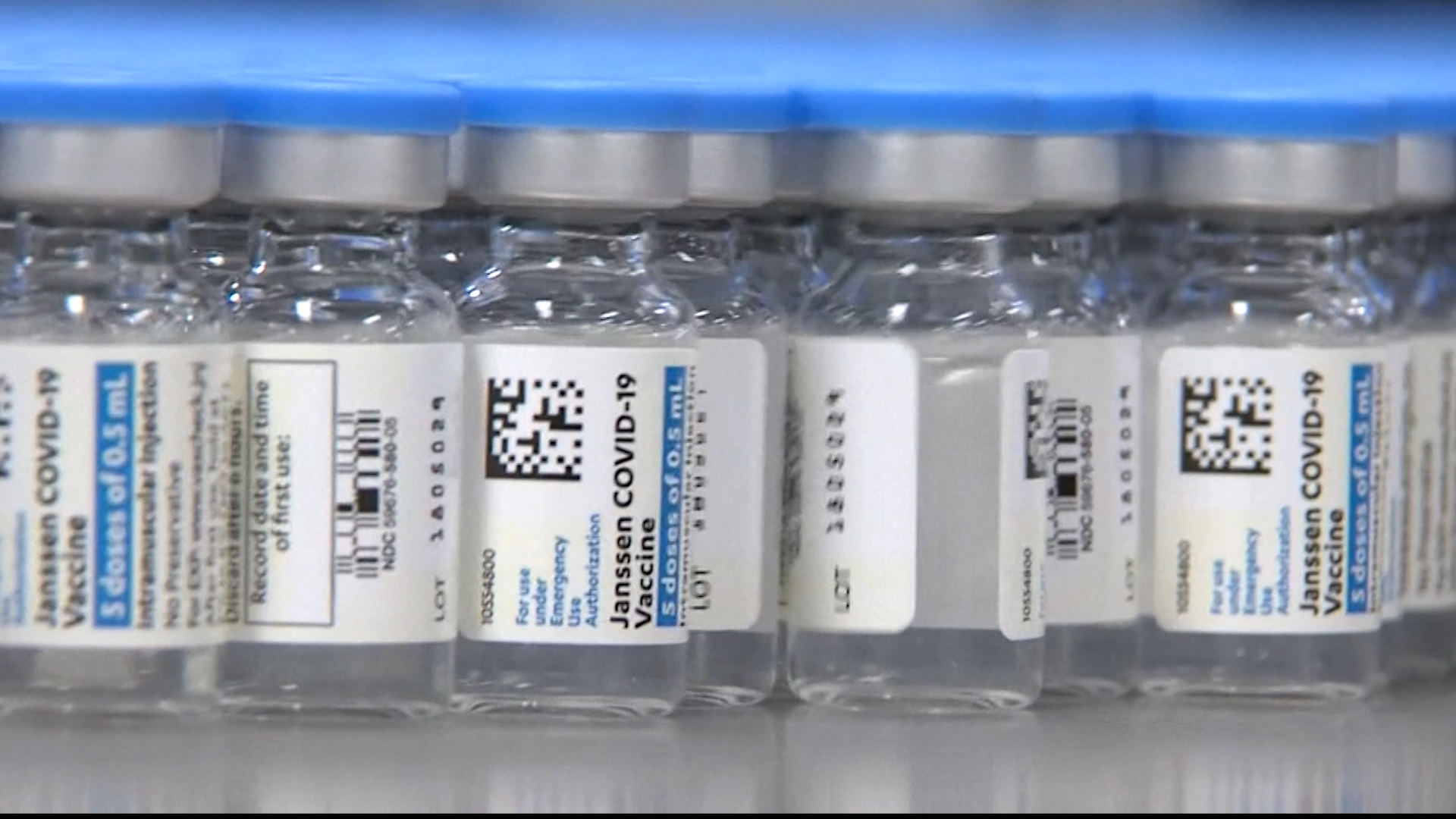
Amid reports of some Johnson & Johnson vaccine recipients developing a rare and potentially dangerous neurological reaction, what can you expect if you're planning to get the one-shot vaccine or already have?
Here's a breakdown of everything we know so far about the J&J vaccine:
How effective is the Johnson & Johnson vaccine?
The FDA said J&J’s vaccine offers strong protection against what matters most: serious illness, hospitalizations and death. One dose was 85% protective against the most severe COVID-19 illness, in a massive study that spanned three continents — protection that remained strong even in countries such as South Africa, where the variants of most concern are spreading.
Feeling out of the loop? We'll catch you up on the Chicago news you need to know. Sign up for the weekly Chicago Catch-Up newsletter here.
The CDC reports J&J/Janssen vaccine was 66.3% effective in clinical trials at preventing COVID-19 illness in people who had no evidence of prior infection 2 weeks after receiving the vaccine.
"The vaccine had high efficacy at preventing hospitalization and death in people who did get sick," the CDC notes. "No one who got COVID-19 at least four weeks after receiving the J&J/Janssen vaccine had to be hospitalized."
While the overall effectiveness data may suggest the J&J candidate isn't quite as strong as the two-dose Pfizer and Moderna options, all of the world’s COVID-19 vaccines have been tested differently, making comparisons nearly impossible, CNBC reported.
There has been concerns surrounding emerging variants of the COVID-19 virus.
So far, studies suggest that all the vaccines currently in use in the U.S. can recognize the emerging variants — but they may not provide as much protection against the new strains.
As the delta variant continues to spread, experts are continuing to push for more Americans to get the COVID vaccine. All three of the vaccines currently authorized under EUA's by the FDA, including Pfizer, Moderna and Johnson & Johnson, have shown to be largely effective against preventing serious illness and death due to COVID, and all three companies say that their vaccines are showing promise in preventing those outcomes with the delta variant as well.
According to a press release earlier this month, the single-shot Johnson & Johnson COVID vaccine provides at least eight months of immunity against coronavirus, and shows “strong, persistent” protection against the delta variant.
“Today’s newly announced studies reinforce the ability of the Johnson & Johnson COVID-19 vaccine to help protect the health of people globally,” Dr. Paul Stoffels, Vice Chairman of the Executive Committee and Chief Scientific Officer at Johnson & Johnson, said. “We believe that our vaccine offers durable protection against COVID-19 and elicits neutralizing activity against the Delta variant. This adds to the robust body of clinical data supporting our single-shot vaccine’s ability to protect against multiple variants of concern.”
According to a recent report, Dr. Scott Gottlieb, former FDA commissioner, said that the Johnson & Johnson vaccine appears to be approximately 60% effective against the delta variant.
How is it different from the Pfizer and Moderna vaccines?
The Johnson & Johnson vaccine requires just one dose, while both Pfizer's and Moderna's vaccines are two shots.
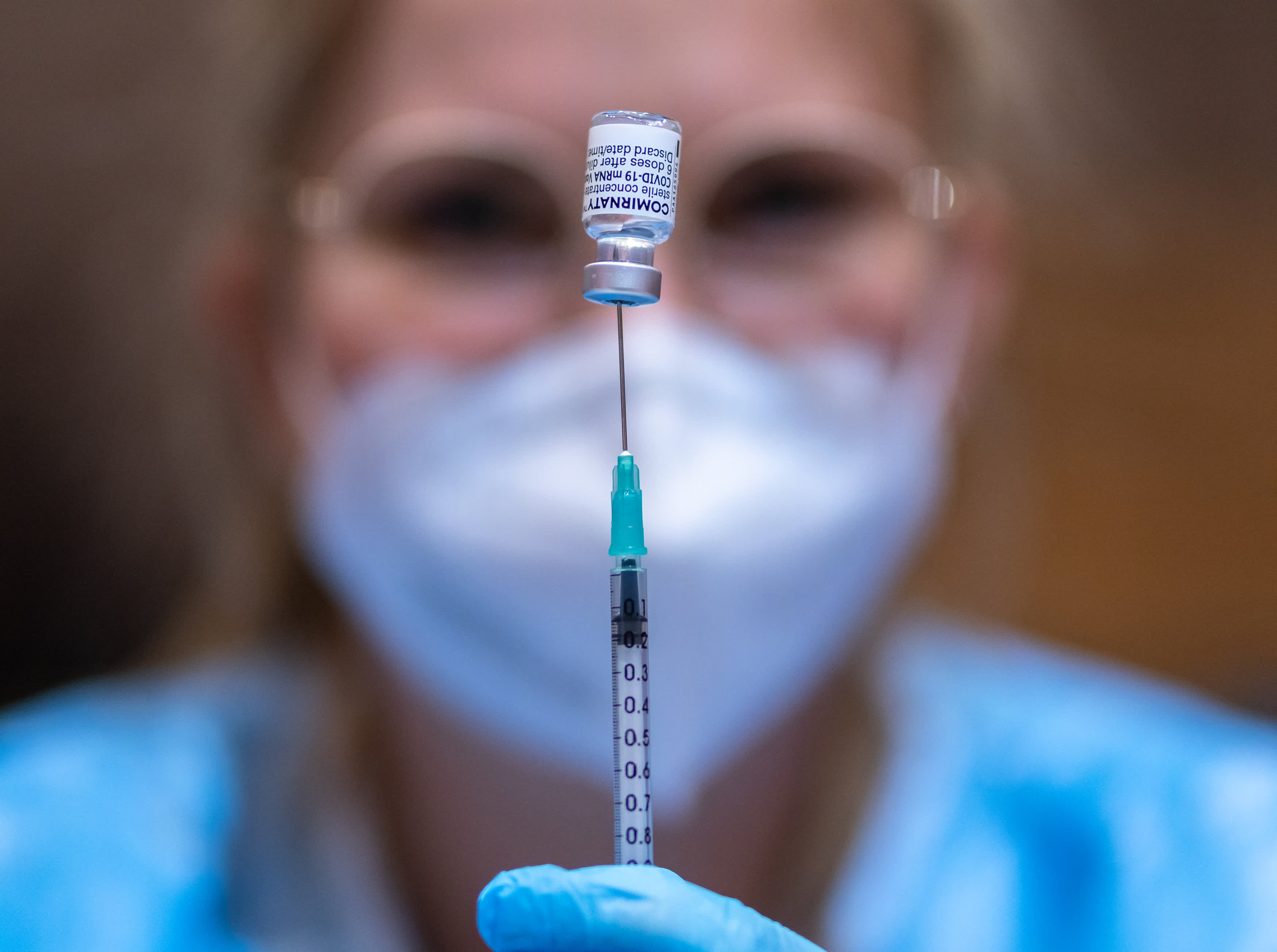
The Pfizer-BioNTech and Moderna vaccines differ from traditional vaccines in their use of mRNA. Instead of introducing a weakened or an inactivated germ into your body, this vaccine injects mRNA, the genetic material that our cells read to make proteins, into your upper arm muscle. It teaches your body how to make the protein that triggers antibody production so if the real virus later enters your body, your immune system will recognize it, according to the federal Centers for Disease Control and Prevention.
Unlike the Pfizer and Moderna shots, the J&J and another vaccine, AstraZeneca, which is not yet authorized for emergency use in the U.S., use a cold virus, called an adenovirus, to carry the spike gene into the body. J&J uses a human adenovirus to create its vaccine while AstraZeneca uses a chimpanzee version.
J&J’s shot uses a cold virus like a Trojan horse to carry the spike gene into the body, where cells make harmless copies of the protein to prime the immune system in case the real virus comes along. It’s the same technology the company used in making an Ebola vaccine.
The Pfizer and Moderna vaccines must also be kept frozen, while the J&J shot can last three months in the refrigerator, making it easier to handle. AstraZeneca's vaccine, which has not yet been approved in the U.S., is made similarly and also requires refrigeration but takes two doses.
What are the common side effects for the J&J vaccine?
Like Pfizer and Moderna's COVID-19 vaccines, the main side effects of the J&J shot are pain at the injection site and flu-like fever, fatigue and headache. These side effects usually start within a day or two of getting the vaccine, according to the CDC.
The CDC reports the most common side effects for all three authorized vaccines is at the injection site. They include:
- Pain
- Redness
- Swelling
Common side effects in the body include:
- Tiredness
- Headache
- Muscle pain
- Chills
- Fever
- Nausea
What about other potential side effect associated with the vaccine, such as Guillain-Barre syndrome?
On Monday, the Food and Drug Administration announced the new warning, flagging reports of Guillain-Barre syndrome, an immune system disorder that can cause muscle weakness and occasionally paralysis. Health officials described the side effect as a “small possible risk" for those getting the shot.
The action comes after the FDA and the Centers for Disease Control and Prevention reviewed reports of about 100 people developing the syndrome after receiving the one-dose vaccine. Almost all of them required hospitalization and one person died, the FDA said.
Guillain-Barre syndrome occurs when the body’s immune system mistakenly attacks some of its nerve cells, causing muscle weakness and sometimes paralysis that typically is temporary. An estimated 3,000 to 6,000 people develop the syndrome each year, according to the CDC. Most people fully recover.
The number of cases reported in connection with J&J's vaccine represents a tiny fraction of the nearly 13 million Americans who have received the one-dose shot. Most cases were reported in men — many 50 years old and up — and usually about two weeks after vaccination.
J&J said in a statement it has been discussing the reports with the FDA and other health regulators around the world.
The CDC said it would ask its panel of outside vaccine experts to review the issue at an upcoming meeting.
The Johnson & Johnson vaccine was also paused for 11 days in April following reports of an extremely rare blood clot known as cerebral venous sinus thrombosis.
U.S. health officials uncovered 15 vaccine recipients who developed a highly unusual kind of blood clot out of nearly 8 million people given the J&J shot. All were women, most under age 50. Three died, and seven remain hospitalized.
But ultimately, federal health officials decided that J&J's one-and-done vaccine is critical to fight the pandemic — and that the small clot risk could be handled with warnings to help younger women decide if they should use that shot or an alternative.
Vaccines historically provide broad protection with little risk but come with occasional side effects just like other drugs and medical therapies. The three COVID-19 vaccines used in the U.S. were each tested in tens of thousands of people, but even such huge studies can’t rule out extremely rare side effects.
The CDC and the FDA have been monitoring side effect reports submitted by physicians, drugmakers and patients to a federal vaccine safety database.
The Wall Street Journal reported Tuesday, citing unnamed sources, that Johnson & Johnson and AstraZeneca are conducting early-stage research into whether potential modifications of their vaccines could reduce or eliminate the risk of rare, but serious, blood clots associated with the shots.
In a statement to CNBC, J&J said it supports "continued research and analysis as we work with medical experts and global health authorities."